Colpocleisis
|
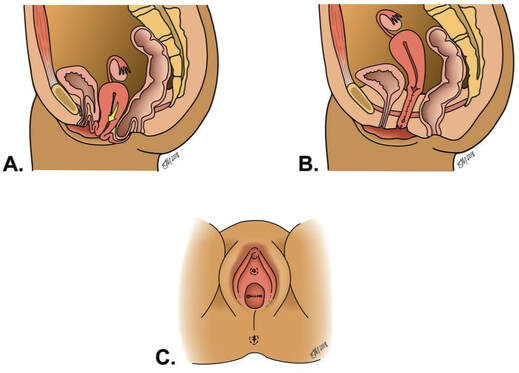
A colpocleisis (vaginal closure procedure) is a surgical treatment option for pelvic organ prolapse in which the length of the vaginal canal is shortened and narrowed so that the prolapsing vagina cannot protrude. This surgery and recovery are swift.
After this surgery, the vagina will be very short and narrowed, making it impossible to have penetrative vaginal intercourse. Obviously, this is not a good treatment option for women who want to be sexually active with penetrative vaginal intercourse. However, the surgery does not change the appearance or function of the clitoris or labia. How Is the Surgery Performed? At Northwestern Medicine, your urogynecologist will perform a colpocleisis through the vagina. It is considered “natural orifice surgery,” so you will not have any incisions on your abdomen. This procedure is the lowest risk surgical procedure available for the repair of prolapse. It can be done quickly under regional (spinal) or general anesthesia, making it an attractive option for women who have medical problems and are not good candidates for more extensive surgeries. In this procedure, the length of the vaginal canal is shortened by sewing the front and back walls of the vagina together, and the size of the opening of the vagina (introitus) is reduced. This effectively reduces vaginal prolapse and prevents further development of prolapse. However, because the vagina is permanently shortened after surgery, women can no longer have sexual intercourse with vaginal penetration. Colpocleisis can be performed on women who have undergone a previous hysterectomy or those who still have a uterus. In rare cases, a hysterectomy can be performed at the time of colpocleisis. How Successful Is This Surgery?
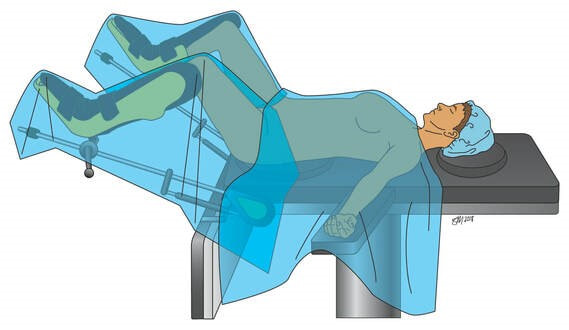
Colpocleisis is very effective and has long-term success rates around 95 percent. Many clinical research studies demonstrate that colpocleisis is safe and effective, even in women who are elderly or have medical problems. Most women are highly satisfied after the procedure. Special considerations before colpocleisis: This procedure cannot be reversed, and it is important to understand that vaginal penetration will not be possible after this procedure. Also, if you have not undergone a hysterectomy either before or at the time of your colpocleisis, your cervix and uterus could develop problems in the future that will be more difficult to assess after this procedure. Depending on your age and gynecologic history, your doctor may recommend a uterine biopsy or ultrasound prior to this surgery. What Is the Recovery? Uterosacral ligament suspension, sacrospinous ligament suspension, and colpocleisis are all vaginal procedures and have similar recoveries. Since your urogynecologist can perform these surgeries utilizing a minimally invasive approach, you will most likely be ready to go home on the day of surgery. To help you accomplish this goal, we have worked with our anesthesiology team to develop an Enhanced Recovery After Surgery (ERAS) program which is designed to minimize postoperative pain, nausea, and fatigue and get you back to your baseline function quickly. We appreciate that you are undergoing surgery to restore your quality of life. Thus, we would like to get you doing the things you want to do as quickly as possible postoperatively. We ask you to abstain from sexual intercourse for at least six weeks while the stitches in your vagina are healing. Otherwise, you can return to your normal activities as soon as you feel ready. How Should I Prepare for Surgery? You will meet with your surgeon as well as our nurse pre-operatively to discuss specific instructions to follow before and after surgery. About Vaginal Surgeries Vaginal surgeries are minimally invasive procedures that require no incisions in the abdomen because access to all of the pelvic organs is obtained using incisions in the vagina. For these procedures, patients are positioned on their backs with legs and feet in supportive stirrups. Other vaginal surgeries include: |
To Request an Appointment
If you're suffering from a pelvic floor disorder, you don't have to live with the symptoms. To learn about treatment options, call 312.694.7337 to schedule an appointment with one of our urogynecologists. Other Vaginal Surgeries for Pelvic Organ Prolapse
MEET OUR TEAM
Our transdisciplinary team works together to ensure that each patient receives a tailored and highly individualized plan of care. |